Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
Advertisement
Pediatric Research (2026)
Structural inequities in neonatal care may influence human milk (HM) feeding outcomes. We examined whether allied health service (AHS) availability differs between safety-net (sn) and non-snNICUs and its association with HM use at discharge among very low birth weight (VLBW) infants.
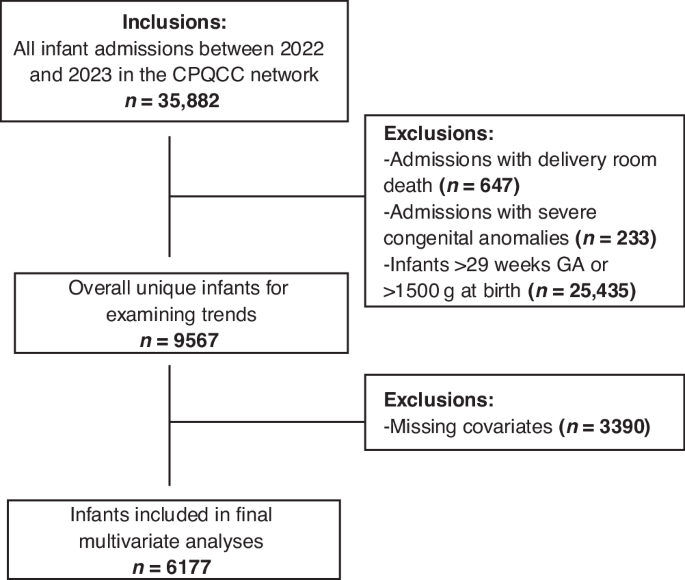
Population-based cohort study of California Perinatal Quality Care Collaborative (CPQCC) data (2022–2023) for infants born <29 weeks’ gestation or <1500 g birth weight (BW). Multivariable models assessed associations between AHS availability (lactation, occupational/physical therapy, social work, psychology) and HM use at discharge, adjusting for infant, maternal, and hospital factors.
Among 138 NICUs, 35% were snNICUs; 64% of VLBW infants were discharged home. AHS availability did not differ between sn and non-snNICUs. Individual AHS availability was not associated with increased HM use, while greater cumulative AHS availability was associated with lower HM use. HM use at discharge was higher in non-snNICUs (70.2% vs. 63.1%, p < 0.001). Higher infant gestation, BW, Apgar score, maternal Asian race, absence of infection and prenatal care were positive predictors; maternal Black and Hispanic race were negative predictors.
Cumulative NICU AHS availability was not associated with higher HM use. Structural presence of AHS alone may not reflect integration into effective feeding practices.
This statewide analysis examined relationships between allied health service (AHS) availability and human milk (HM) nutrition among preterm infants in California NICUs.
Contrary to expectations, AHS availability did not differ between safety-net and non–safety-net hospitals.
Individual AHS availability showed no association with HM use at discharge, while greater cumulative AHS availability correlated with lower HM use.
Findings challenge assumptions that more AHS automatically improves HM outcomes and highlight the need to evaluate how allied health resources are integrated, coordinated, and aligned with family-centered lactation support in the NICU.
This is a preview of subscription content, access via your institution
Subscribe to this journal
Receive 14 print issues and online access
276,54 € per year
only 19,75 € per issue
Buy this article
39,95 €
Prices may be subject to local taxes which are calculated during checkout
The data that support the findings of this study are derived from the California Perinatal Quality Care Collaborative (CPQCC) database. Due to data use agreements and protections for patient privacy, these data are not publicly available. De-identified data may be made available to qualified investigators upon reasonable request and subject to approval by CPQCC through a formal data request process. Information on data access requests can be found at https://www.cpqcc.org or by contacting CPQCC directly.
Liu, J. et al. Racial and ethnic disparities in human milk intake at neonatal intensive care unit discharge among very low birth weight infants in California. J. Pediatrics 218, 49–56 (2020).
Article Google Scholar
Goldstein, G. P. et al. Racial/ethnic disparities and human milk use in necrotizing enterocolitis. Pediatr. Res. 88, 3–9 (2020).
Article PubMed PubMed Central Google Scholar
Parker M. G., et al. Addressing disparities in mother’s milk for VLBW infants through statewide quality improvement. Pediatrics. 144, e20183809 (2019).
Meek J. Y., Noble L. Policy statement: breastfeeding and the use of human milk. Pediatrics. 150, https://doi.org/10.1542/peds.2022-057988 (2022).
Rose, A. T. et al. US state policies for Medicaid coverage of donor human milk. J. Perinatol. 42, 829–834 (2022).
Article PubMed PubMed Central Google Scholar
Liu, J. et al. Evaluating care in safety net hospitals: clinical outcomes and neonatal intensive care unit quality of care in California. J. Pediatrics 243, 99–106.e3 (2021).
Article Google Scholar
Belfort, M. B. et al. Diet, weight gain, and head growth in hospitalized US very preterm infants: a 10-year observational study. Am. J. Clin. Nutr. 109, 1373–1379 (2019).
Article PubMed Google Scholar
Hefner J. L., Hogan T. H., Opoku-Agyeman W., Menachemi N. Defining safety net hospitals in the health services research literature: a systematic review and critical appraisal. BMC Health Services Res. 21, https://doi.org/10.1186/s12913-021-06292-9 (2021).
Werner, R. M., Goldman, L. E. & Dudley, R. A. Comparison of change in quality of care between safety-net and non–safety-net hospitals. JAMA 299, 2180 (2008).
Article CAS PubMed Google Scholar
Morales, L. S. et al. Mortality among very low-birthweight infants in hospitals serving minority populations. Am. J. Public Health 95, 2206–2212 (2005).
Article PubMed PubMed Central Google Scholar
Patel, A. L., Johnson, T. J. & Meier, P. P. Racial and socioeconomic disparities in breast milk feedings in US neonatal intensive care units. Pediatr. Res. 89, 344–352 (2020).
Article PubMed PubMed Central Google Scholar
Lussier, M. M. et al. Independent predictors of human milk receipt at neonatal intensive care unit discharge. Am. J. Perinatol. 31, 891–898 (2013).
Article PubMed Google Scholar
Godsil, J. L. et al. Breastfeeding interventions for dyads with medical complexity: a mixed methods study. Open J. Occup. Ther. 13, 1–18 (2025).
Article Google Scholar
Orton, J. L., Olsen, J. E., Ong, K., Lester, R. & Spittle, A. J. NICU graduates: the role of the allied health team in follow-up. Pediatr. Ann. 47, e165–e171 (2018).
Article PubMed Google Scholar
Muirhead, R. & Bates, A. Does the implementation of multidisciplinary developmental care rounds increase the utilization of developmental caregiving interventions in the neonatal unit? J. Perinat. Neonatal Nurs. 37, 153–163 (2023).
Article PubMed Google Scholar
Çömük B. N., Takçi S., Seren H. C. Improving feeding skills and transition to breastfeeding in early preterm infants: a randomized controlled trial of oromotor intervention. Front. Pediatrics. 11, https://doi.org/10.3389/fped.2023.1252254 (2023).
Ravi, D., Iacob, A. & Profit, J. Unequal care: racial/ethnic disparities in neonatal intensive care delivery. Semin. Perinatol. 45, 151411 (2021).
Article PubMed PubMed Central Google Scholar
Pai, V. V. et al. Improved referral of very low birthweight infants to high-risk infant follow-up in California. J. Pediatrics 216, 101–108.e1 (2020).
Article Google Scholar
Padula, A. M. et al. Multilevel social factors and NICU quality of care in California. J. Perinatol. 41, 404–412 (2020).
Article PubMed PubMed Central Google Scholar
Edwards, E. M., Ehret, D. E. Y., Soll, R. F. & Horbar, J. D. Vermont Oxford Network: a worldwide learning community. Transl. Pediatrics 8, 182–192 (2019).
Article Google Scholar
Gould, J. B. Building the first statewide quality improvement collaborative, the CPQCC: a historic perspective. Children 7, 177 (2020).
Article PubMed PubMed Central Google Scholar
Danielsen, B. H., Carmichael, S. L., Gould, J. B. & Lee, H. C. Linked birth cohort files for perinatal health research: California as a model for methodology and implementation. Ann. Epidemiol. 79, 10–18 (2023).
Article PubMed PubMed Central Google Scholar
Profit J. et al. Racial/ethnic disparity in NICU quality of care delivery. Pediatrics. 140 (2017).
Karvonen, K. L. et al. Structural racism is associated with adverse postnatal outcomes among Black preterm infants. Pediatr. Res. 94, 371–377 (2023).
Article PubMed Google Scholar
Razdan, S., Hedli, L., Sigurdson, K., Profit, J. & Morton, C. Disparity drivers, potential solutions, and the role of a health equity dashboard in the neonatal intensive care unit: a qualitative study. J. Perinatol. 44, 659–664 (2024).
Article PubMed Google Scholar
Sankar, M. N. et al. Barriers to optimal breast milk provision in the neonatal intensive care unit. J. Perinatol. 42, 1076–1082 (2022).
Article PubMed Google Scholar
Elgersma,K. M., Davis, J. A., Mohan-ONeill, S., Overpeck, S. R. & Desai, H. Breastfeeding infants with CHD: an evidence summary andrecommendations from the Cardiac Newborn Neuroprotective Network, a special interest group of the CardiacNeurodevelopmental Outcome Collaborative. Cardiol Young. 2053–2066 (2025).
Parker M. G. et al. Promoting human milk and breastfeeding for the very low birth weight infant. Pediatrics. 148, e2021054272 (2021)
Almalki M., Gildea A., Boyle B. Parents’ experiences of family-centred care in neonatal intensive care units: a qualitative thematic synthesis. J. Neonatal Nurs. 21, (2025).
Abugov H., Ochoa Marín S. C., Semenic S., Arroyave I. C. Barriers and facilitators to breastfeeding support practices in a neonatal intensive care unit in Colombia. Investigación y Educación en Enfermería. 39, https://doi.org/10.17533/udea.iee.v39n1e11 (2021).
Lee J. Neonatal family-centered care: evidence and practice models. Clin. Exp. Pediatrics. 67, https://doi.org/10.3345/cep.2023.00367 (2023).
Leeman, K. T. et al. Improving access to lactation consultation and early breast milk use in an outborn NICU. Pediatr. Qual. Saf. 4, e130 (2019).
Article PubMed PubMed Central Google Scholar
Download references
We thank the California Perinatal Quality Care Collaborative (CPQCC) and its member hospitals for providing access to de-identified clinical data used in this study. We are deeply grateful to Dr. Jochen Profit for his mentorship and guidance throughout the conceptualization and analysis of this work.
This work was conducted under the mentorship of Dr. Jochen Profit, whose research program is supported by the National Institutes of Health (NIH) [grant number, R01MD01817302]. No direct financial support was received for this analysis.
Department of Pediatrics, Division of Neonatal-Perinatal Medicine, Stanford University School of Medicine and Lucile Packard Children’s Hospital at Stanford, Palo Alto, CA, USA
Igbagbosanmi Olatunji & Jochen Profit
California Perinatal Quality Care Collaborative, Stanford University School of Medicine, Palo Alto, CA, USA
Jessica Liu & Jochen Profit
PubMed Google Scholar
PubMed Google Scholar
PubMed Google Scholar
Igbagbosanmi Olatunji conceptualized the study, contributed to data analysis and interpretation, and drafted the initial manuscript. Jessica Liu conducted the statistical analyses and contributed to data interpretation. Jochen Profit provided mentorship, conceptual guidance, and critical review of the manuscript for important intellectual content. All authors reviewed and approved the final version of the manuscript as submitted and agree to be accountable for all aspects of the work.
Correspondence to Igbagbosanmi Olatunji.
The authors declare no competing interests.
Patient consent was not required as this study used de-identified data from the California Perinatal Quality Care Collaborative (CPQCC) registry.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Reprints and permissions
Olatunji, I., Liu, J. & Profit, J. Allied health services availability and human milk nutrition among preterm infants. Pediatr Res (2026). https://doi.org/10.1038/s41390-026-04939-z
Download citation
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41390-026-04939-z
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
Advertisement
Pediatric Research (Pediatr Res)
ISSN 1530-0447 (online)
ISSN 0031-3998 (print)
© 2026 Springer Nature Limited